Pediatric High-Grade Gliomas
What are pediatric high-grade gliomas?
Pediatric high-grade gliomas (pHGGs) are a form of brain tumor found in children. They arise from glial cells, also known as the “connective glue”, which are the supportive cells of the brain. This form of glioma is considered to be “high-grade” because of its fast-growing, aggressive, and malignant nature. Types of pHGGs include diffuse midline glioma, diffuse hemispheric glioma, and diffuse pediatric‐type high‐grade glioma.
pHGGs are most common in children between 15 and 19 years old.
Unfortunately, we do not yet know the exact cause of pHGGs. However, they are believed to arise from cancer-promoting mutations within glial progenitor cells, including oligodendrocyte progenitor cells during development. Healthy glial cells function to support and maintain neurons in the brain. However, when mutated, they can lose their function and begin proliferating uncontrollably. In diffuse midline gliomas, the cancer-promoting mutation occurs within the gene encoding the H3 histone. Histones are proteins that play a crucial role in gene regulation. Without a properly functioning H3 histone, there is uncontrolled gene expression of genes that were once turned off, which can promote tumor growth. Additionally, the environment within the brain surrounding the tumor can also affect and support tumor growth. Laboratories around the world are working to understand more about the origins of pHGGs in greater detail.
Why are pHGGs difficult to treat?
Pediatric high-grade gliomas, like other tumors, are able to rapidly proliferate, resulting in aggressive tumor growth within the brain. pHGGs have leaky blood vessels supplying them and they have an abnormal microenvironment, meaning there are few stable pathways for treatment. pHGGs also go undetected by the immune system, making them difficult for the immune system to attack and naturally destroy. Furthermore, pHGGs have a high presence of tumor-associated macrophages, a type of immune cell that would normally attack the tumor but instead gets tricked by the tumor to suppresses the immune response and help the tumor grow.
pHGGs are responsible for the most brain cancer-related deaths in children.
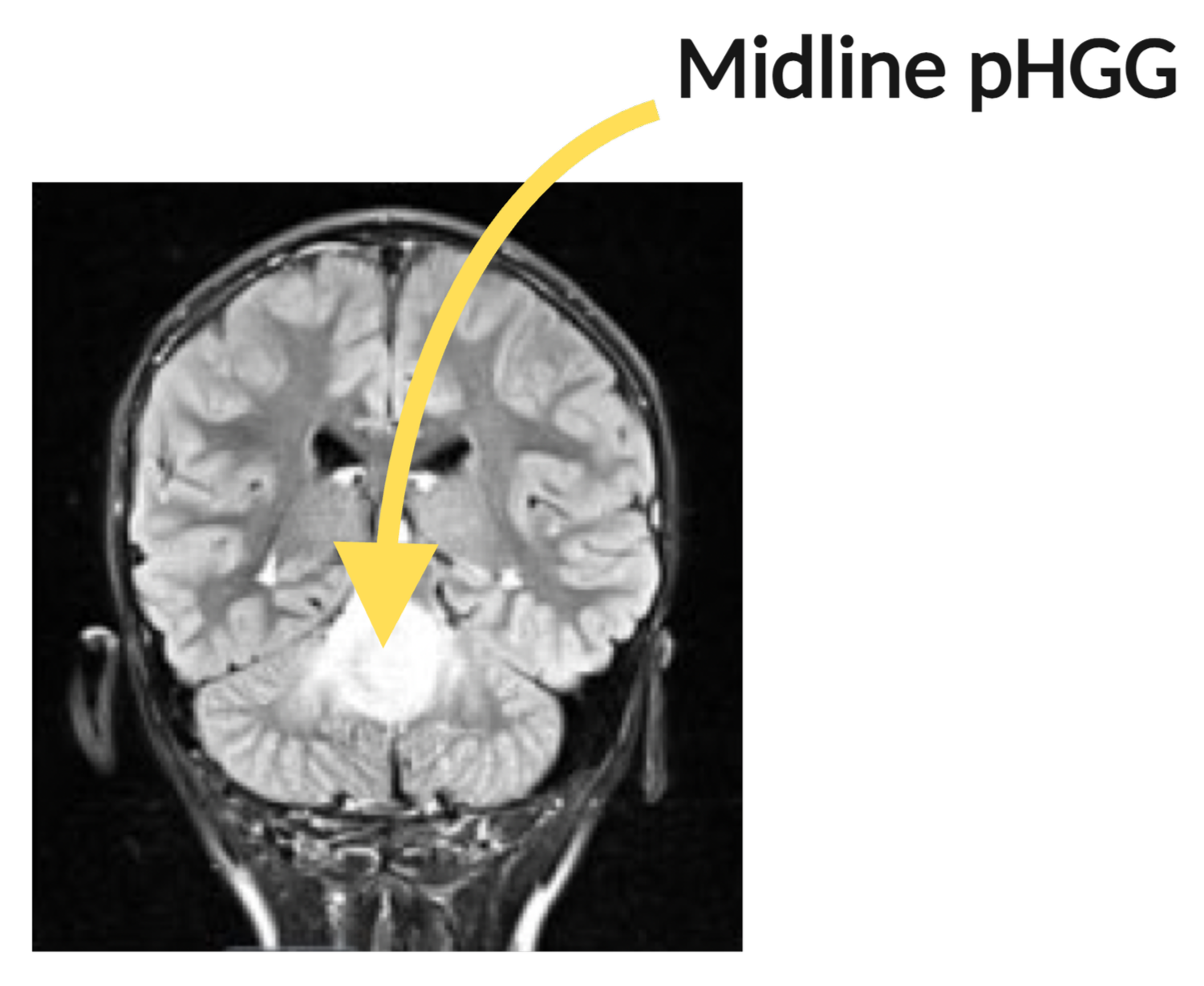
Where do pHGGs come from?
pHGG facts and statistics:
pHGGs do not often spread, or metastasize, outside of the central nervous system (brain and spinal cord).
Around 500 children in the U.S. are diagnosed with pHGG every year.
pHGGs make up 10% of pediatric brain tumors.
After a pHGG diagnosis, the average survival ranges from 10 to 73 months.
Depending on the tumor’s size, location, and many other biological factors, pHGG symptoms can vary. Some typical symptoms include:
Headache
Vomiting
Seizures
Fatigue
Motor weakness
Difficulty walking and balancing
Created in https://BioRender.com
What symptoms are associated with pHGGs?
Pediatric high-grade gliomas requires unique diagnostic testing. Through various imaging strategies, biopsies, and molecular testing physicians can accurately diagnose pHGG subtypes in patients.
Radiation and chemotherapy are the standard of care for pHGGs. Unfortunately, there are not many other effective therapeutic options for pHGGs. Due to the location of pHGGs within the brain, surgical removal is risky, and the natural protective barrier known as the blood brain barrier prevents most therapeutics from getting to the tumor. When attempting to treat pHGGs, medical professionals often create a personalized regimen based on the patient’s unique tumor, resulting in a strategy that tends to be a combination of multiple treatments.
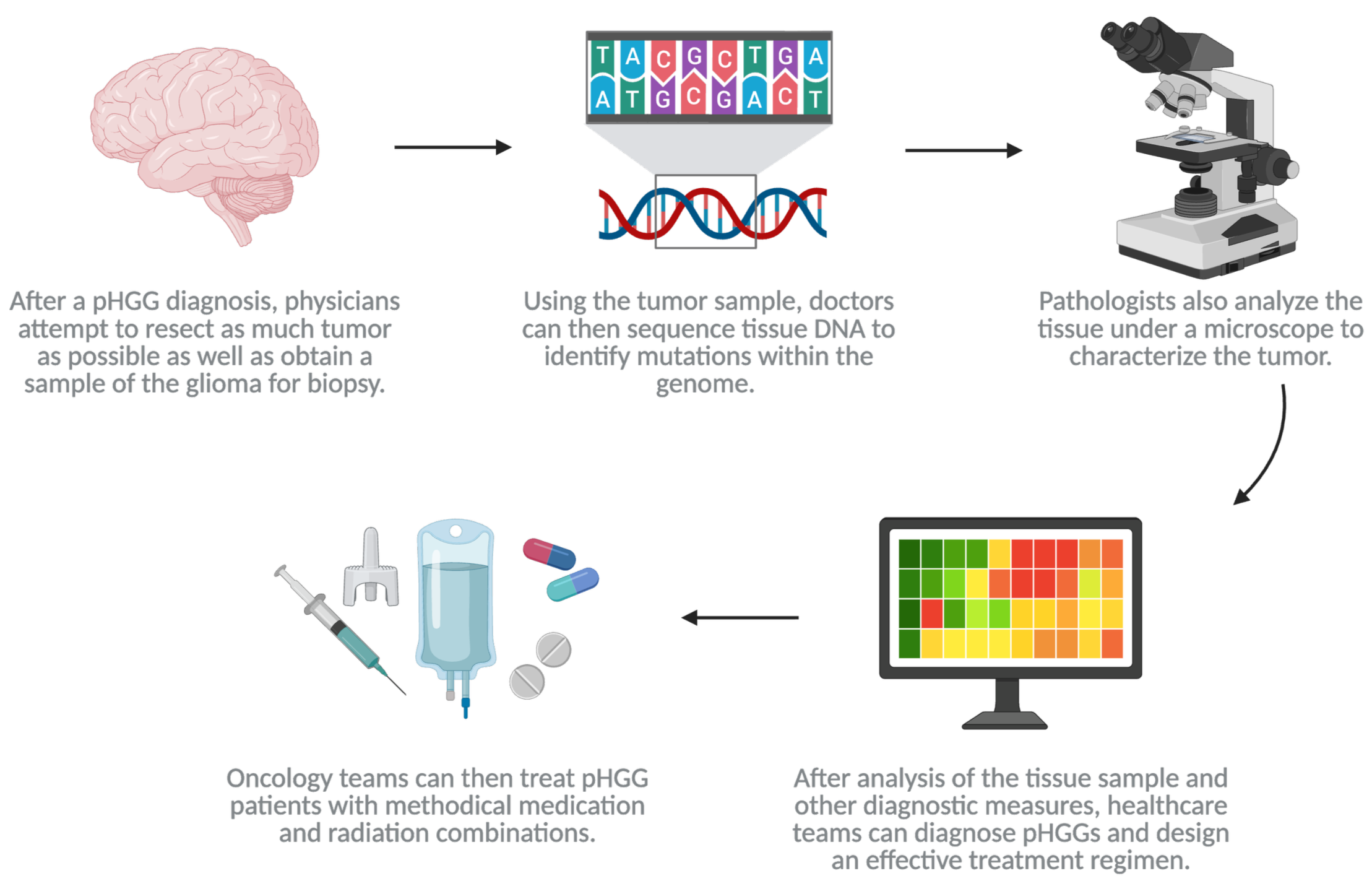
pHGG diagnosis and treatments:
Created in https://BioRender.com
The Ross Lab’s research aims to uncover more about pHGGs and the associated immune response to help improve pHGG treatment for patients. We are heavily focused on identifying the next generation of therapeutic targets by combining relevant experimental models and utilizing human data.
Support resources:
Despite the uncertainty of a pediatric cancer diagnosis, in addition to the support provided by psychologists, social workers, and child life specialists, there are numerous online resources designed to help pediatric cancer patients and their families. For example, the COG Family Handbook is a comprehensive handbook from the Children's Oncology Group that provides families with reliable, expert-reviewed information about treatment, support, and long-term care for children with cancer.
Financial Assistance
The National Children's Cancer Society: Provides financial, emotional, and educational support to families affected by pediatric cancer, including transportation assistance, emergency funds, and one-on-one case manager support.
Family Reach: Helps families facing a cancer diagnosis afford everyday needs like food, housing, transportation, and utilities through various grants, financial education, and assistance in resource navigation.
The Andrew McDonough B+ Foundation: Provides financial assistance and support to families facing childhood cancer, including virtual support groups, school re-entry resources, and educational webinars.
CancerCare: Offers financial assistance for cancer-related costs such as transportation and childcare, with oncology social workers available to help families find additional resources.
Compass to Care: Removes financial and logistical barriers with regard to travel for treatment by funding transportation costs, including gas, rideshares, flights, and lodging.
National Pediatric Cancer Foundation: Funds pediatric cancer clinical trials and offers a Health Navigator program to connect families with educational resources and personalized guidance about their child's cancer diagnosis.
Support for Patients & Families
Alex’s Lemonade Stand: Offers families an extensive resource directory, travel assistance for clinical trials, sibling support programs, free guides, and a resource navigator to help connect families with the support resources they need.
The American Childhood Cancer Organization: Provides free support, educational resources, and a national network of support groups to children with cancer, their families, and survivors.
Austin Hatcher Foundation: Provides free, lifelong psychological and rehabilitative care for families affected by childhood cancer, including mental health therapy, occupational therapy, educational advocacy, and family programs.
Mattie Miracle Cancer Foundation: Supports the psychological, social, and emotional needs of children with cancer and their families, advocating for higher standards of care and funding child life specialists, therapy grants, and wellness programs.
CureSearch: Funds pediatric cancer research with the goal of developing safer, more effective treatments, and provides educational resources and support to help families navigate cancer diagnoses.
pHGG clinical trials:
Laboratories, hospitals, and organizations around the world are working to discover effective treatments for pHGGs.
| Clinical Trial | Status | Location(s) | Link |
|---|
The information provided above is not medical advice. For questions and concerns, please contact a healthcare professional.
Worsened coordination
Vision problems
Confusion
Memory loss
Behavioral changes
Cognitive changes

Created in https://BioRender.com